Suyash was standing with a distressed face by the window of his room as he watched the other boys of his colony play football. He is a 7 year old and his parents can’t afford to allow him outdoor activities since he is suffering from haemophilia.
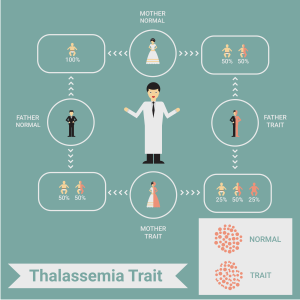
Haemophilia is not just a single disease, but rather one of a group of inherited genetic bleeding disorders that cause abnormal or exaggerated bleeding and poor blood clotting. This is most commonly used to refer to two specific conditions known as haemophilia A and haemophilia B. Haemophilia A and B are inherited in an X-linked recessive genetic pattern and are therefore much more common in males. This pattern of inheritance implies that a given gene on the X chromosome expresses itself only when there is no normal gene present. For example, Suyash has only one X chromosome, so Suyash has the defective gene on his sole X chromosome and so is referred to be homozygous for haemophilia. But does that mean it is impossible for a girl to have haemophilia? Well it is not. A girl can definitely have haemophilia, but she would have to have the defective gene on both of her X chromosomes or have one haemophilia gene as well as lost/defective copy of the second X chromosome. Now if a girl has one copy of the defective gene on one of her X chromosomes and a normal second X chromosome, she does not have haemophilia but is referred to as heterozygous for haemophilia. Her male offspring will have a 50% chance of inheriting the one mutated X gene and hence have a 50% chance of inheriting haemophilia from their carrier mother.
Occurrence rate
Haemophilia is by far the most common X-linked genetic disease. Haemophilia A happens in about 1 out of every 5000 live male births. Haemophilia A and B occur in all racial categories. Haemophilia A is about five times more common than B. Haemophilia B has an occurrence rate of 1 out of 20-30,000 live male births.
History or Origin
Haemophilia was acknowledged in ancient times. The Talmud, a collection of Jewish rabbinical writings of the second century AD, mentioned that male babies should not be circumcised provided two brothers had already died due to excessive bleeding from the operation. The Arabic physician Albucasis, who lived in the 12th century, described a family with males who died from bleeding after minor injury.
John Conrad Otto, a physician from Philadelphia wrote in 1803, “An account of haemorrhagic disposition existing in certain families.” He clearly acknowledged the cardinal features of haemophilia, i.e., an inherited tendency of males to bleed. But the first use of the word “haemophilia” was found in an essay written in 1828 from the University of Zurich.
Haemophilia is called the royal disease, as several members of European royal families were affected by this disease, inherited from Queen Victoria of England (1837 to 1901), who was a haemophilia B carrier. Her eighth son Leopold contracted haemophilia B, suffered from frequent haemorrhages and died of a brain haemorrhage at the early age of 31. Two of Queen Victoria’s daughters, Alice and Beatrice, were the carriers of haemophilia B and transmitted the disease on to the Spanish, German, and Russian royal families.
What causes Haemophilia?
Blood platelets coagulate at the wound site, forming a clot. The process, known as “the coagulation cascade” normally stops bleeding. Then the body’s clotting factors work together to create a more permanent plug in the wound. Haemophilia is an inherited genetic condition, meaning it is passed down through families. It is caused by a defect in the gene that determines how the body makes factors VIII, IX, or XI. These genes are located on the X chromosome, thus making haemophilia an X-linked recessive disease.
Each individual inherits two sex chromosomes from their parents. Females have two X chromosomes, which they inherit from each parent. Males have one X chromosome (from their mothers) and one Y chromosome (from their fathers). Since the genetic defect that causes haemophilia is located on the X chromosome, fathers can’t pass the disease to their sons.
A female who has the altered gene on one of her X chromosomes is called a “carrier.” This means she may pass the disease to her kids but she doesn’t have the disease herself. But, females who are carriers often have an increased risk of bleeding.
Symptoms and diagnosis
There can be some prominent symptoms as well as no symptoms depending on the severity of the disease that is factor deficiency. People with such deficiency suffer from spontaneous bleeding. Spontaneous bleeding can cause the following:
- blood in the urine
- bleeding gums
- large, unexplained bruises
- blood in the stool
- deep bruises
- excessive bleeding
- frequent nosebleeds
- pain in the joints
- tight joints
- irritability (in children)
- Some other severe symptoms include-
- blurred or doubled vision
- extreme sleepiness
- continuous bleeding from an injury
- vomiting repeatedly and neck pain
Haemophilia is usually diagnosed through a blood test. Your doctor will take out a small sample of blood from your vein and measure the amount of clotting factor present. The sample is then graded to determine the severity of the factor deficiency:
- Mild haemophilia: It is indicated by a clotting factor in the plasma that’s between 5% and 40%.
- Moderate haemophilia: It is indicated by a clotting factor in the plasma that’s between 1% and 5%.
- Severe haemophilia: It is indicated by a clotting factor in the plasma of less than 1%.
Treatment
Usually, Haemophilia A is treated through a prescription hormone called desmopressin, which is injected into the vein. This medication works by stimulating the factors responsible for the process of blood clotting.
One can opt for physical therapy for rehabilitation if one’s joints are damaged by haemophilia.
Preventing haemophilia
Haemophilia is a congenital disorder and it can’t be prevented. However, if you opt for in vitro fertilization, they can be tested for the condition and only the eggs without haemophilia can be implanted.
Haemophilia in India
Haemophilia, although rare in India should be given thorough attention due to its severity. Certain organisations like Haemophilia Federation are working for the betterment of children affected by Haemophilia. India doesn’t have a national policy on the prevention and control of genetic disorders. There is scarce data on the epidemiology of other genetic disorders in India. Haemophilia has an incidence of 1 per 10,000 births and occurs as spontaneous or trauma-induced haemorrhagic episodes in patients, leading to chronic disability and premature mortality in untreated patients or patients with sub-optimal treatment (1).
Genetic counseling
Genetic counselors are specialized health care professionals with expertise in medical genetics and psychological counseling. They help family members by facilitating informed decision making regarding their genetic health. By assessing medical and family history they help in identifying underlying genetic causes of diseases, guide in management of symptoms and provide information to at-risk relatives.
Genetic testing and genetic counseling for an individual or a child suspected to have haemophilia could be beneficial for the following reasons:
- Accurate diagnosis of the disease by identifying the underlying genetic causes
- Accurate management of the disease and long-term surveillance
- Predicting risk for at-risk family members
- Couples can opt for prenatal genetic testing or preimplantation genetic diagnosis to make an informed decision about the pregnancy
- Receive psychological support to cope with the implications of the disease
Speaking with a genetic counselor can help you to better understand possible underlying genetic causes and discuss emotional and medical implications for yourself and your family members. A genetic counselor is a specialized health care professional who has expertise in medical genetics and psychological counseling. If you would like to set up a genetic counseling appointment CALL US on 1800 102 4595 (toll-free) or 040-66986700or WRITE TO US at info@mapmygenome.in.

Works cited
1. Kar A, Phadnis S, Dharmarajan S, Nakade J. Epidemiology & social costs of haemophilia in India. Indian J Med Res. 2014;140(1):19–31.