Dyslipidemia is the presence of unusual amounts of lipids (cholesterol, triglycerides, or fat phospholipids) in the bloodstream. These blood lipids are fatty substances that are maintained normally through a balanced diet and healthy lifestyle. Dyslipidemia is a major risk factor for heart diseases like coronary artery disease and stroke. Long-term research studies have proven that individuals with healthier lifestyles and few risk factors for coronary heart disease are less likely to develop any type of heart disease. Prevention and proper management of dyslipidemia can help reduce the morbidity and mortality associated with cardiovascular diseases.
Dyslipidemia is of the following common forms.
- High levels of low-density lipoprotein (LDL)/bad cholesterol leads to accumulation of fats in the arteries.
- Low levels of high-density lipoprotein (HDL) good cholesterol helps in the removal of LDL from the blood.
- High levels of triglycerides (TGA)
- High cholesterol, which equates to high triglyceride and LDL levels
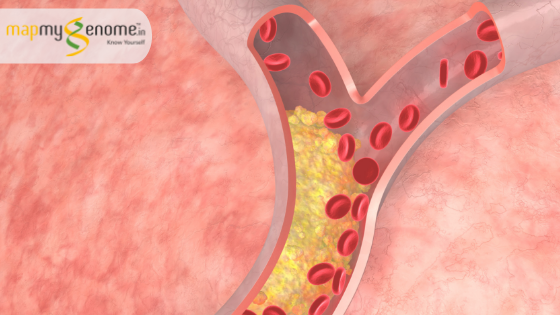
Normal and healthy lipid levels in the blood differ from person to person, and individuals with high levels of LDL/TGA or extremely low HDL levels have greater chances of acquiring atherosclerosis. Atherosclerosis occurs when fatty deposits called plaques build up in the blood vessels and obstruct free flow of blood. Over time, these plaques accumulate heavily and lead to grave conditions like heart attacks and strokes.
How Common Is It?
Dyslipidemia is a major risk factor for atherosclerosis in India. Research reports suggested that cholesterol levels are high in 25–30% of urban and 15–20% of the rural population. Comparably, the prevalence is not greater than it is in the high-income countries. Borderline high LDL cholesterol, low HDL cholesterol, and high triglycerides are the most frequent types of dyslipidemia in the country. Recent case-control studies revealed that there’s a remarkable association between coronary events with elevated LDL cholesterol, total cholesterol, apolipoprotein B, and non-HDL cholesterol and inverse association with high apolipoprotein A and HDL cholesterol. Incidentally, there’s little evidence of dyslipidemia, available treatment procedures, and preventive measures of hypercholesterolemia in the country. Management of dyslipidemia at a clinical level can be advanced with quality physical education, availability of medicines, and increased awareness of self-management of cholesterol. (Gupta, Rajeev, et al, 2017).
(Source: http://publish.uwo.ca/~tcheung8/Lipids.html)
Clinical Features:
- Pain or tightness and pressure in the chest, neck, jaw, shoulders, and back
- Dizziness
- Palpitations in the heart
- Trouble in breathing
- Cold sweat
- fainting
- Heartburn, vomiting, and nausea
- Swelling in legs, ankles, feet, stomach, and neck veins.
Note: Many people with dyslipidemia do not have any symptoms. A Lipid Profile test may help in screening.
Dyslipidemia – Risk Factors and Complications:
- Sedentary lifestyle and lack of regular physical activity
- Obesity
- Usage of alcohol, tobacco, and illicit drugs
- Type II diabetes
- Chronic kidney and liver conditions
- Foods high in saturated fats and trans fats
- Family history
- Old age
Do Genes Have Anything To Do With It?
HDL Cholesterol:
Genetic variation in LPL results in dysregulation of lipid metabolism and processing of triglycerides. The NUTF2 gene is a key element of nuclear protein transport — import into and export out of the cell’s nucleus. The CETP gene product facilitates the uptake of HDL-c particles by the liver, thereby regulating circulating HDL-c levels. Genetic variation in and near LIPG (Endothelial lipase) inhibits enzyme function, which may increase HDL-c levels.
LDL Cholesterol:
The Apolipoprotein family of genes such as APOB (Apolipoprotein B) and APOC1 (Apolipoprotein C1) are known to influence LDL-c concentration in the body. Genetic variations in these genes or their regulatory regions cause hypercholesterolemia and particularly increase plasma LDL-c levels. Individuals carrying LDLR (Low-Density Lipoprotein Receptor) gene variants may have lower levels of bad cholesterol (LDL-c) in the body and may have a reduced risk for heart disease.
Triglyceride Levels:
Variants near the MLXIP (regulates glycolysis and lipogenesis) gene, in the GALNT2 gene (involved in oligosaccharide synthesis), and in the 11q23 region (near the ZNF259 gene and the APOA5-A4-C3-A1 gene complex) are associated with elevated triglyceride levels.
Fat Sensitivity:
PPARG — peroxisome proliferator-activated receptor-gamma — gene variation affects sensitivity to dietary fat. The gene regulates caloric intake/expenditure, weight regulation, energy balance, and adipose metabolism.
(Source: https://www.doctorshealthpress.com/food-and-nutrition-articles/dyslipidemia-diet-foods-to-eat-guidelines-to-follow/)
Managing Dyslipidemia Risk — Diet and Lifestyle:
Treatment of dyslipidemia should focus on preventing atherosclerotic cardiovascular disease (ASCVD). This includes coronary syndromes, transient ischemic attack and stroke, and peripheral arterial disease. Treatment for dyslipidemia should be targeted at controlling hypertension and diabetes, smoking cessation, etc. Lifestyle modifications include regular exercise, decrease in weight, and abstinence from consumption of concentrated sugars and alcohol. Foods like whole egg, egg yolk, spinach, chicory greens, avocado, and apple can have positive effects on a dyslipidemia patient.
How Can Mapmygenome Help You:
At Mapmygenome, our focus is on predictive risk assessment, maintaining a proper diet, and adapting to a healthier lifestyle. A comprehensive wellness assessment like Genomepatri will give an insight into the weaknesses of your immunity, genetic predisposition to specific health conditions, drug efficiency and helps in pre-empting most of these risks. Genetic counselling is therefore recommended to obtain authenticated reviewing, testing/screening options, diet/lifestyle interventions, and educational and emotional support.
Tapping into your genes will assist you to know the real ‘YOU’. Genomepatri helps you find the best-suited route for yourself, and reiterates the importance of not following the crowd but forging a unique way of leading quality life. It is personalized, predictive, participatory, preventive, and POWERFUL!!!
References:
- Gupta, Rajeev, et al. “Recent trends in the epidemiology of dyslipidemias in India.” Indian heart journal 69.3 (2017): 382-392.
- Joshi, Shashank R., et al. “Prevalence of dyslipidemia in urban and rural India: the ICMR–INDIAB study.” PloS one 9.5 (2014): e96808.
- Kopin, Laurie, and Charles J. Lowenstein. “Dyslipidemia.”Annals of internal medicine 167.11 (2017): ITC81-ITC96.




