In our previous blog, COVID-19 antibody testing and ELISA (Part 1), we discussed the benefits of COVID antibody testing and why ELISA is a preferred method for the same. In Part 2 (this is VERY science-y!), we shall learn about the steps in an ELISA procedure, interpretation and limitations.
The ELISA Procedure :
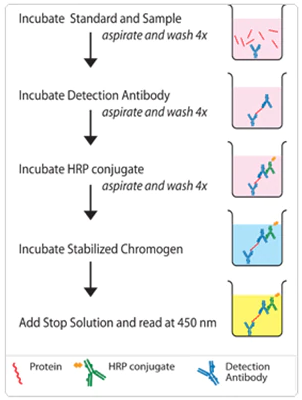
There are six main steps in ELISA – antibody coating, protein capture, detection antibody, enzyme conjugate, addition of substrate and analysis.
- Antibody coating: the specific antibodies are added into a 96-wells ELISA plate and are immobilized on high-protein binding plates by overnight incubation (4°C ).
- Protein capture: standard dilution solutions are added to the wells after a certain series of wash (after washing off the non specific binding proteins from the wells) and capture the bound antibodies
- Detection antibodies: specific dilution buffers are added to dilute the detection antibodies for the detection of captured proteins.
- Enzyme conjugate: the enzyme-labelled secondary antibodies are added to the wells after a series of dilution of the enzyme-labelled secondary antibodies with the sample dilution buffer and left for incubation for 1hr at 37℃ for the binding of secondary antibodies to the primary antibody.
- Addition of substrate: after removing the secondary antibodies through a series of wash, colorimetric substrate is added to the wells to obtain the colored solution in the wells when catalysed by enzymes.
- Analysis: the absorbance is measured in an ELISA reader at 450nm.
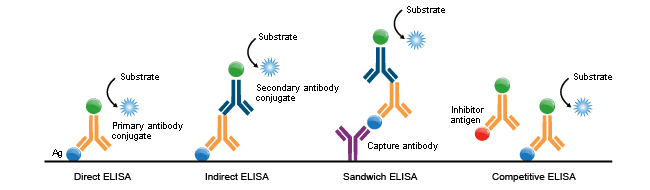
Based on the lipoprotein (antigen) – target antibody binding, the assay can be of four types – Direct ELISA, Indirect ELISA, Sandwich, Competitive ELISA.
- Direct ELISA: The target protein is immobilized on the surface of the microtiter plate and incubated with the enzyme labelled target antibody, and is recognised by the enzyme conjugate that allows the detection after the substrate reactions.
- Indirect ELISA: The target protein is immobilized on the surface of plate and incubated with the target antibodies(primary antibody), followed by the secondary antibody that conjugates with the primary antibody, the activity is then measured on the plate after the substrate reaction. Labelled secondary antibodies are commercially available.
- Sandwich ELISA: Two antibodies specific to two different epitopes on the antigens are used. An antibody (primary antibody) is immobilized with the target protein(antigen) first on the surface of the plate first, and to another target specific antibody(secondary antibody) at different epitopes on the antigen. After the substrate reaction the activity can be measured.
- Competitive ELISA: An antibody specific to the target antigen(reference antigen) is immobilized at the surface of the microtiter plate, and incubated with the sample( inhibitor antigen) containing the target proteins, it competes with the reference antigen for binding to primary antibody. Unbound materials are washed away, the more antigen in the sample, the less specific antibody bound to the coated antigen, lighter the color of solution in wells and lower the final signal. Conversely, when the antigen is low in the sample, the level of antibody-bound enzyme-labeled antigen is higher, darker the colour of solution in the wells and higher the final concentration.
Also Read: COVID-19 antibody testing and ELISA (Part 1)
Ig ELISA :
The ELISA is a useful and suitable method for quantification of immunoglobulins of all isotypes and specificities. Using isotype-specific antibodies, the amounts of IgG, IgA, IgM, and IgE (released into the blood during the immune reactions) in the samples can be quantified.
The development of monoclonal antibodies specific to the isotype-determining regions of immunoglobulins helps increase the specificity of detection. A sandwich ELISA method can be used, in which the plate has been coated with antibody that captures the immunoglobulins and also determines the total amount of immunoglobulins (irrespective of antigen specificity). These antigen-specific immunoglobulins bind to coated antigen and can be detected by using the biotin labelled antibodies.
Antibodies directly conjugated to an enzyme are available commercially, that determine the total levels of IgG, IgA, or IgM in the samples. For measurement of total IgE, the use of biotin labelled detection antibody in combination with a streptavidin–enzyme conjugate is recommended for increased sensitivity.
Using the IgG ELISA in parallel with the IgM ELISA , one can observe the relative variations in the antibodies in the given sample. The IgG-ELISA is less subjective to immunofluorescence and a large number of samples can be processed at a time.
IgG ELISA test for COVID-19:
This test measures the IgG antibodies (produced as a part of immune response to the infection) using the plasma or serum samples collected from the individuals. The IgG solid-phase ELISA is designed to measure the amount of target proteins bound to the matched antibody pair. The target specific antibody is pre-coated , samples,standards and controls are added to wells for immobilization(capture) of the antibodies.
Potential benefits and risks involved:
There are certain benefits and risks associated with the test. One of the main benefits is that the test results shows if a person is infected with the virus or not, thereby limiting the spread of the disease. The test also benefits as it helps identify the infected people who are asymptomatic. The test can benefit the healthcare worker – doctors, nurses etc, the test can also help your health care provider, inform you of your health conditions, and give the possible recommendations.
The potential risks involved with the test are – you may have possible discomfort or bruising, infection or any other complications that may happen during or after the sample collection Serious complications are very rarely seen. The test may also show false results.
What does a positive test result mean?
The positive result for COVID ELISA IgG antibody test indicates the presence of IgG antibodies in the sample and the individual was exposed to the virus. The presence of IgG antibodies indicates a past infection. IgG antibodies develop later than IgM antibodies following the infection, and generally do not appear until 7 – 10 days after the infection. It is still unknown how long the IgG antibodies will remain in the body after infection and if they confer immunity to infection.
There are still chances that these antibodies developed in the body indicate past infection due to other viruses/bacteria etc. The laboratory test results should always be considered, in the context of clinical observations and epidemiological data prior to making a final diagnosis and also in patient management decisions. There are also chances that the test results are incorrect (false positive). However, in the event of a false positive result, risks to an individual could include the risk of infection by exposure to persons with active COVID-19.
What does a negative result mean?
The negative test results for COVID ELISA IgG antibody test indicates the specific antibodies were not present in the sample collected. However, the negative test results do not rule out previous COVID-19. The test results should not be used as the sole basis for treatment, patient management decisions, or to rule out active infection because some patients tested during the early stages of infection may not develop the IgG antibodies despite the active infection and not all individuals develop a detectable IgG response.
The possibility of false negative results should be considered in the context of a patient’s recent exposures and the presence of clinical signs and symptoms.
References
- https://pib.gov.in/PressReleasePage.aspx?PRID=1622766
- https://timesofindia.indiatimes.com/gadgets-news/pune-lab-develops-made-in-india-covid-19-kit-that-can-test-90-samples-in-2-5-hours/articleshow/75668541.cms
- https://www.fda.gov/media/136151/download
- https://www.cdc.gov/coronavirus/2019-ncov/symptoms-testing/testing.html
- https://www.fda.gov/media/137030/download